When dealing with immunosuppressants, drugs that intentionally reduce or block immune system activity. Also known as immune suppressive agents, they become necessary whenever the body’s own defenses threaten a medical goal.
Corticosteroids, synthetic versions of the hormone cortisol, act fast to calm inflammation and immune activation are often the first line after surgery or during an acute flare. Their quick effect makes them ideal for induction therapy, but long‑term use demands low dosing to avoid bone loss, diabetes, or weight gain. Calcineurin inhibitors, agents such as cyclosporine and tacrolimus that block a specific signaling enzyme in T‑cells provide deeper suppression for organ‑transplant patients. Monitoring blood levels is critical because the therapeutic window is narrow and kidney toxicity is a real risk.
Beyond these, Biologic agents, engineered proteins that target specific immune pathways like TNF‑α or IL‑6 have reshaped treatment of rheumatoid arthritis, psoriasis, and inflammatory bowel disease. Their precision reduces broad‑scale immune shutdown, yet cost and infection risk keep them reserved for patients who don’t respond to older drugs. Understanding how immunosuppressants work helps patients and clinicians balance effectiveness with safety.
Immunosuppressants encompass multiple drug families, each with distinct mechanisms, side‑effect profiles, and monitoring needs. They require careful laboratory testing—liver enzymes for corticosteroids, trough levels for calcineurin inhibitors, and infection screening for biologics. Failure to follow protocols can lead to organ rejection, disease flare, or severe complications.
Autoimmune diseases influence immunosuppressant choice because the underlying pathology dictates which immune pathways are most harmful. For example, lupus patients often need a combination of steroids and antimetabolites, while transplant recipients rely heavily on calcineurin inhibitors to prevent graft loss. Matching the drug to the disease ensures the right amount of suppression without unnecessary toxicity.
Organ transplant is perhaps the most classic scenario for immunosuppressant use. After a kidney or liver transplant, a life‑long regimen of a calcineurin inhibitor, an antimetabolite, and low‑dose steroids is common. The goal is to keep the new organ alive while minimizing drug‑related damage. Patients must stay vigilant about infections, blood pressure, and kidney function—regular follow‑up visits become a routine part of life.
The articles below dive deeper into specific drugs, compare alternatives, and offer real‑world tips for dosing, side‑effect management, and cost‑saving strategies. Whether you’re starting a new regimen or looking to switch agents, the collection provides the practical insight you need to make informed decisions.

Echinacea may seem like a safe immune booster, but for people on immunosuppressants, it can interfere with life-saving medications. Learn why experts warn against using it after transplants or for autoimmune conditions.
Immunosuppressants prevent organ rejection after transplant but carry serious risks like infection, cancer, and kidney damage. Learn how to manage these drugs safely, avoid missed doses, and reduce long-term side effects.
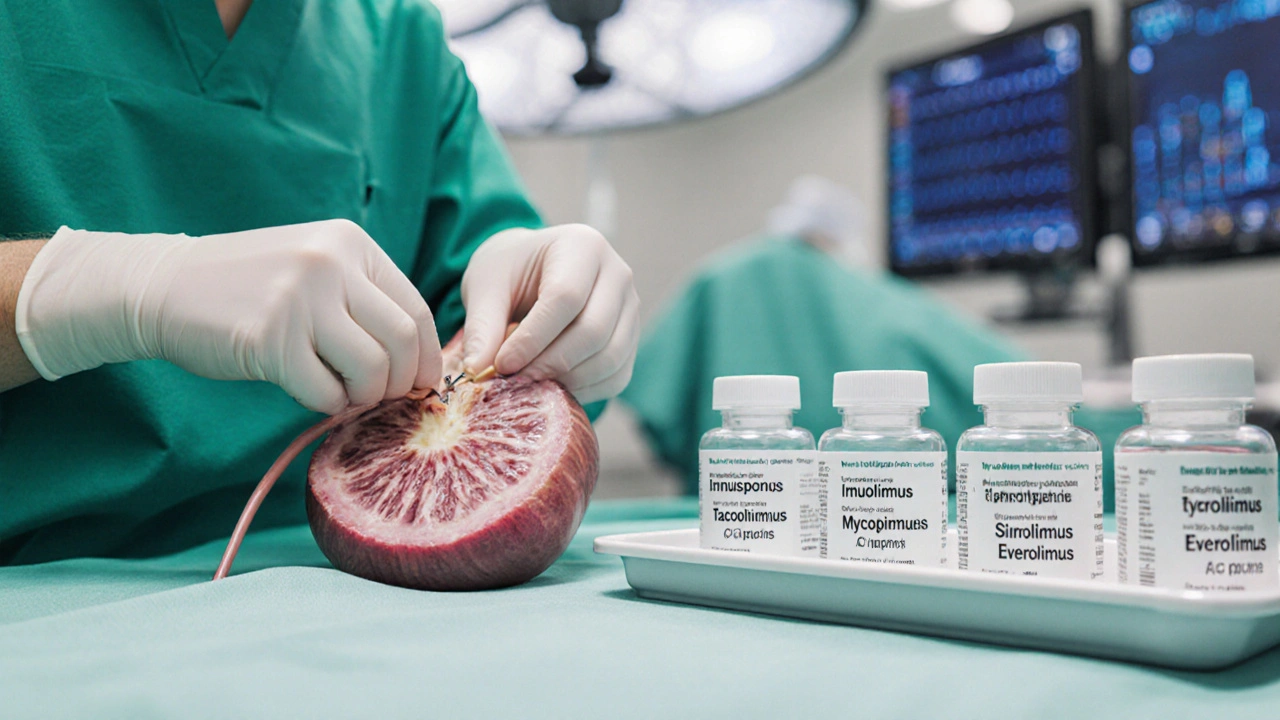
A side‑by‑side look at Imusporin (cyclosporine) versus tacrolimus, mycophenolate, sirolimus, everolimus and others, covering mechanisms, side effects, UK costs and when to switch.

Curious about chlorella? Get an evidence-based look at its nutrition, real benefits, safe dosage, side effects, and how to choose a clean, quality supplement.

Tired of Pharmex Direct or just curious about what else is out there? This article unpacks the best alternatives for Canadians looking for reliable pharmacy options. From big-brand stores to convenient online choices, get the details on pricing, services, and trustworthiness. For anyone who wants straightforward pharmacy solutions without the fuss, this will make picking your next pharmacy a whole lot easier.

The best time to take statins isn't about night or morning-it's about consistency. Learn how statin timing affects side effects and cholesterol lowering, and why adherence beats clock time.

A clear comparison of Cleocin Gel (clindamycin) with other topical acne treatments, covering how they work, price, side effects, and tips for choosing the best option.
Explore the rise of direct-to-consumer generic pharmacies and how new business models are bypassing PBMs to lower drug prices and improve patient access.