When coronary artery disease, a condition where plaque builds up in the arteries that supply blood to the heart. Also known as coronary heart disease, it’s the most common type of heart disease and the top cause of death worldwide. It happens when fatty deposits—called plaque—slowly clog the arteries around your heart. Over time, that blockage cuts off oxygen and nutrients your heart needs to pump properly. You might not feel anything at first, but when the blockage gets bad enough, it can trigger chest pain, shortness of breath, or even a heart attack.
What causes this buildup? High cholesterol, a waxy substance in your blood that can stick to artery walls is a big player, especially the bad kind (LDL). But blood pressure, the force of blood pushing against artery walls that stays too high for too long also damages the lining of your arteries, making it easier for plaque to stick. Smoking, diabetes, lack of movement, and too much salt all make it worse. You don’t need to be old to get it—many people in their 40s and 50s are already developing early signs without knowing it.
There’s no magic fix, but you can slow it down—or even reverse it—by changing what you eat, how much you move, and what meds you take. Statins lower cholesterol. Blood pressure pills like ramipril reduce strain on your heart. Aspirin can help prevent clots. And lifestyle changes? They’re not optional. Walking 30 minutes a day, cutting out processed foods, and quitting smoking do more than any pill alone. The good news? Most people with coronary artery disease live full lives when they stay on top of it.
Below, you’ll find real-world guides on how medications like ramipril affect your salt intake, how to manage drug interactions, how to store pills safely, and what alternatives exist when side effects become a problem. These aren’t theoretical articles—they’re practical tools for people living with this condition every day.
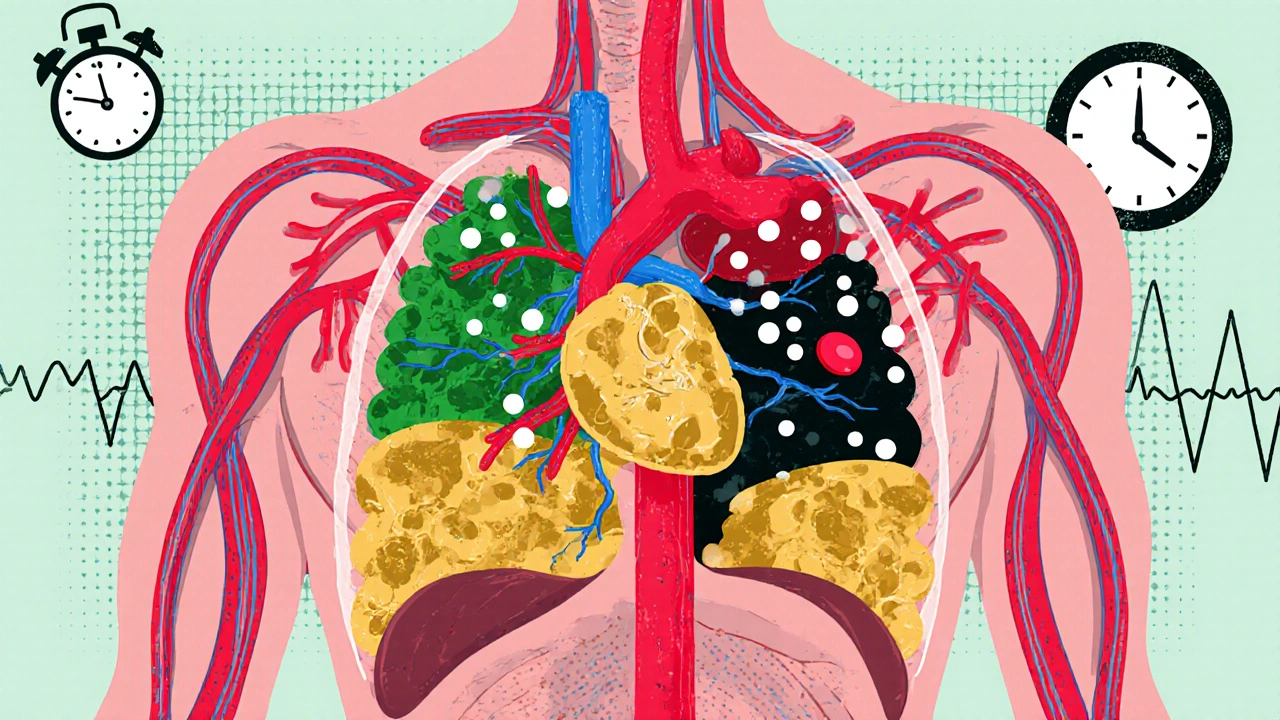
Coronary artery disease, caused by atherosclerosis, is the leading cause of death worldwide. Learn how plaque builds up, who’s at risk, and what treatments actually work-based on the latest 2023 guidelines.

A practical guide comparing Modvigil (modafinil) with armodafinil, adrafinil, Provigil and caffeine‑L‑theanine, covering cost, duration, safety and best use cases.
Biosimilars are the closest thing to generics for complex biologic drugs. They're highly similar, FDA-approved, and can save patients up to 60% on costs. Learn how they work, why they're not exact copies, and how to use them safely.

Governments don't set prices for generic drugs - they let competition do it. Learn how FDA approvals, FTC enforcement, and market forces keep generic medications affordable without direct price controls.

The nocebo effect explains why people feel side effects from medications even when the drug has no active ingredient. Expectations, not chemistry, often drive these reactions - and they're more common than you think.

Switching to generic medications can be safe - but for drugs with a narrow therapeutic index, even small changes in absorption can cause serious effects. Learn when dose adjustments are needed and how to protect yourself.