The goal of managing this transition is simple: maintain the clinical success of the treatment while cutting down the monthly pharmacy bill. However, moving from a brand-name drug to any generic can be stressful. Patients often worry about whether the "cheaper version" works as well. When dealing with authorized generics, those worries are largely unfounded because the chemistry is identical. Let's look at how to handle this switch without the stress.
Why Authorized Generics Differ from Standard Generics
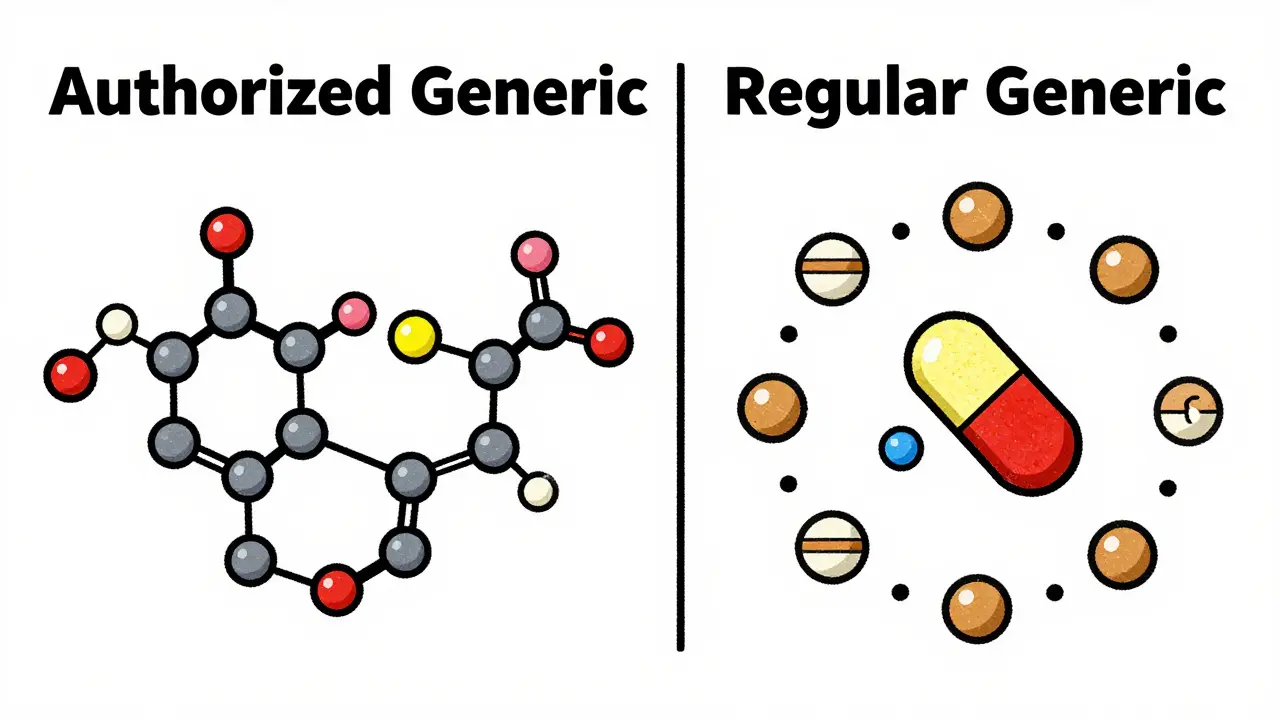
To understand the transition, you first have to understand what you're switching to. Most people think all generics are the same, but there is a big difference between a standard generic and an authorized one. A regular generic is made by a different company that proves to the FDA is the United States Food and Drug Administration, the federal agency responsible for protecting public health by ensuring the safety and efficacy of medications that their version is bioequivalent. This means it works the same way, but the inactive ingredients-like fillers, dyes, or binders-can vary.
Authorized generics are different. They are produced by the original brand-name manufacturer or a licensee using the exact same formula and often the same factory. This means the active and inactive ingredients are identical. For a person sensitive to certain dyes or lactose, this is a game-changer. Data from GoodRx shows that while about 12.7% of patients struggle with inactive ingredients when moving to regular generics, that number drops to just 2.3% with authorized versions.
| Feature | Authorized Generic | Regular Generic |
|---|---|---|
| Manufacturer | Brand-name company (or licensee) | Third-party generic manufacturer |
| Ingredients | Identical active & inactive ingredients | Same active; different inactive ingredients |
| FDA Approval | Marketed under original NDA | Requires ANDA approval |
| Switchback Rate | Lower (approx. 7.2%) | Higher (approx. 18.4%) |
Managing Narrow Therapeutic Index Drugs
For some medications, a tiny change in dosage or formulation can be dangerous. These are known as Narrow Therapeutic Index (NTI) drugs medications where a small difference in dose or blood concentration can lead to a significant change in the drug's effect or toxicity . If you are taking a blood thinner or certain seizure medications, you fall into this category. In these cases, switching to a regular generic can sometimes cause "therapeutic failure" because of slight variations in how the drug is absorbed.
This is where authorized generics shine. Because they are identical to the brand, they provide a stability that regular generics sometimes lack. Studies indicate a 28% lower incidence of therapeutic failure when patients switch to authorized generics compared to regular ones. If you're on an NTI drug, the transition requires more caution. The American Medical Association suggests enhanced monitoring for the first 90 days after the switch to ensure your body is responding correctly.
The Practical Steps for a Smooth Transition
You shouldn't just swap pills at the pharmacy counter. A coordinated effort between your doctor and pharmacist ensures nothing falls through the cracks. Here is the most effective way to handle the move:
- Check Availability: Not every drug has an authorized generic. Use tools like the FDA's Orange Book or the 'Authorized Generic Finder' to see if one exists for your medication.
- Audit Insurance Costs: This is the tricky part. Sometimes insurance companies place authorized generics in a higher "tier" than regular generics. You might find that the "brand-identical" version actually costs you more in copays. Always verify the price before switching.
- Education and Visuals: Talk to your pharmacist about the composition. Knowing that the pill is chemically identical-even if the color or marking is slightly different-helps reduce the anxiety that often leads patients to switch back to the brand.
- The 14-30 Day Check-in: Set a reminder to evaluate how you feel two weeks and one month after the switch. This is the critical window to catch any adverse reactions or a dip in effectiveness.
Overcoming Common Transition Hurdles
The biggest hurdle isn't medical-it's psychological and administrative. Many patients experience the "different pill" effect. When a tablet looks different, the brain sometimes convinces the patient it isn't working, even if the chemistry is the same. This is a major driver behind the 22% of switchbacks seen with regular generics. Because authorized generics are so close to the brand, this psychological barrier is much lower.
Another headache is the electronic health record (EHR) system. Many pharmacy systems don't actually distinguish between a "generic" and an "authorized generic." This can lead to confusion if you move from one pharmacy to another. To avoid this, ask your pharmacist for the exact NDC (National Drug Code) of the medication. This unique number ensures you get the exact same version every time, regardless of the pharmacy's software.

The Financial Impact and Market Reality
Why do companies do this? It's a strategic move. Brand companies launch authorized generics to compete with other generic manufacturers and capture a slice of the lower-cost market. For the patient, this is a win. The Federal Trade Commission has noted that these drugs can reduce retail prices by 4-8% and wholesale prices by 7-14%.
However, be aware that availability is limited. As of late 2023, only about 37.5% of brand-name drugs with generic alternatives actually had an authorized generic version. If you can't find one, it doesn't mean your pharmacist is ignoring you; it likely means the manufacturer hasn't released one.
Is an authorized generic exactly the same as the brand-name drug?
Yes. Authorized generics are manufactured by the same company that makes the brand-name version (or a licensee) using the same active and inactive ingredients. The only differences are typically the label and sometimes the physical markings on the tablet.
Why would I choose an authorized generic over a regular generic?
The main reason is consistency. Regular generics must be bioequivalent but can have different fillers or dyes. If you have sensitivities to certain inactive ingredients or are taking a narrow therapeutic index drug where precision is critical, an authorized generic eliminates the risk of formulation differences.
Will my insurance cover authorized generics?
Most do, but the cost can vary. Some insurance plans treat them as standard generics, while others might place them in a different pricing tier. It is essential to check your specific formulary to ensure you aren't paying more for the authorized version than you would for a regular generic.
How can I tell if my medication is an authorized generic?
You can check the FDA's Orange Book or use the 'Authorized Generic Finder' tool in the Drugs@FDA database. You can also ask your pharmacist to verify the manufacturer and the NDC code of the product.
Are there any risks in switching from brand to authorized generic?
Because they are identical in formulation, the clinical risk is extremely low. However, as with any medication change, it's important to monitor for any changes in how you feel and maintain a coordinated line of communication with your healthcare provider during the first 90 days.
Next Steps for Patients and Providers
If you are a patient looking to save money without sacrificing the quality of your brand-name drug, start by asking your pharmacist: "Is there an authorized generic available for this medication?" If the answer is yes, request a price comparison between the brand, the authorized generic, and the regular generic.
For providers, the best approach is to prioritize authorized generics for your most sensitive patients-those with complex allergies or those on NTI medications. By guiding the patient through a structured 30-day follow-up, you can ensure a successful transition that boosts both patient adherence and financial accessibility.



Sam Hayes
April 4, 2026 AT 10:22just a heads up that you should definitely double check the NDC code with your pharmacist since some systems really do lump them all together
simran kaur
April 4, 2026 AT 20:22Please. As if we are supposed to believe the "brand name company" is just altruistically lowering prices for us. It is a transparent ploy to maintain a monopoly on the market share while pretending to be accessible. They control the supply chain and the formula, and now they want us to trust the same entity that overcharged us for decades. It is absolutely laughable that anyone would think this is about the patient and not about quarterly profit margins for the board of directors. The entire pharmaceutical industrial complex is designed to keep us dependent and compliant through these subtle shifts in labeling. I will stick to a completely different manufacturer if I can find one, because once you give the brand company the "authorized generic" loophole, they own your medical history and your wallet forever. It is just another layer of corporate gaslighting wrapped in a "helpful guide" for the masses who lack the intellect to see the strings being pulled.
Joseph Rutakangwa
April 5, 2026 AT 09:36good point on the ndc codes
Will Baker
April 7, 2026 AT 00:54Oh wow, a guide on how to save a few pennies while still feeding the big pharma machine. How revolutionary. I'm sure the 4% retail price drop will totally change your life while the CEO buys another yacht with the rest of the profits. Truly inspiring stuff here.
Rob Newton
April 8, 2026 AT 20:35Bioequivalence is a myth. Trust the results, not the label.
Mark Zhang
April 9, 2026 AT 23:49It really is a relief for people with sensitive systems. Knowing the inactive ingredients are the same takes a lot of the anxiety out of the process.
Aysha Hind
April 11, 2026 AT 09:11The so-called "authorized" tag is just a fancy linguistic cloak for the same corporate sludge. They're just rearranging the deck chairs on the Titanic and calling it a nautical upgrade. It's a shell game, plain and simple, played with our health as the chips. Who knows what's actually in those fillers when the FDA is essentially a revolving door for pharma lobbyists anyway? Total nonsense.
Jenna Carpenter
April 12, 2026 AT 13:58Some of you just dont get it... its about alignment with your body and the energy of the medicine, not just the label!! you need to look deeper than the chemestry lol
Dee McDonald
April 13, 2026 AT 12:27Let's get this done! Everyone needs to call their pharmacy right now and demand to know if an authorized generic is available for their meds! Stop overpaying for the exact same stuff just because of a logo on the box! Get your NDC codes and take control of your healthcare spending!
The Charlotte Moms Blog
April 14, 2026 AT 08:03The data is skewed... obviously... and the "psychological barrier" is just a way to dismiss actual patient experiences with drug efficacy... typical...!!
Vicki Marinker
April 15, 2026 AT 16:43It is quite tedious to even discuss the merits of this when the systemic failure of healthcare pricing is the actual issue.
HARSH GUSANI
April 16, 2026 AT 20:11My country makes better meds anyway! 🇮🇳 Who cares about these US FDA rules when we have our own systems! 💊💪
Sakshi Mahant
April 17, 2026 AT 19:45It is helpful to see a bridge between the two options for those who are hesitant. Balance is key in these transitions.
Hope Azzaratta-Rubyhawk
April 17, 2026 AT 23:55YOU MUST ENSURE YOUR DOCTOR IS FULLY INFORMED OF THIS SWITCH IMMEDIATELY! There is no room for error when it comes to your health!